For patients who have a clear mechanical or structural cause of hip pain, University of Virginia Health System now offers hip arthroscopy, a minimally invasive surgical approach that provides pain relief without the risks of open surgery. According to orthopedic surgeon Winston Gwathmey, MD, arthroscopy has been widely used for decades to treat conditions of the knee and shoulder; however, hip arthroscopy has been slower to evolve because the hip joint is more complex and less accessible.
“Arthroscopic access to the shoulder and knee joint is relatively straightforward, allowing more rapid development and application of arthroscopic techniques for common injuries of these joints such as rotator cuff tears and ACL tears,” says Gwathmey. “The hip is a deep and tightly congruent ball-and-socket joint rendering arthroscopic access and maneuvering more difficult. However, technical advances over the past two decades have stimulated significant growth in hip arthroscopy and we can now do many things through a scope that previously required open surgery.”
Indications for Surgery
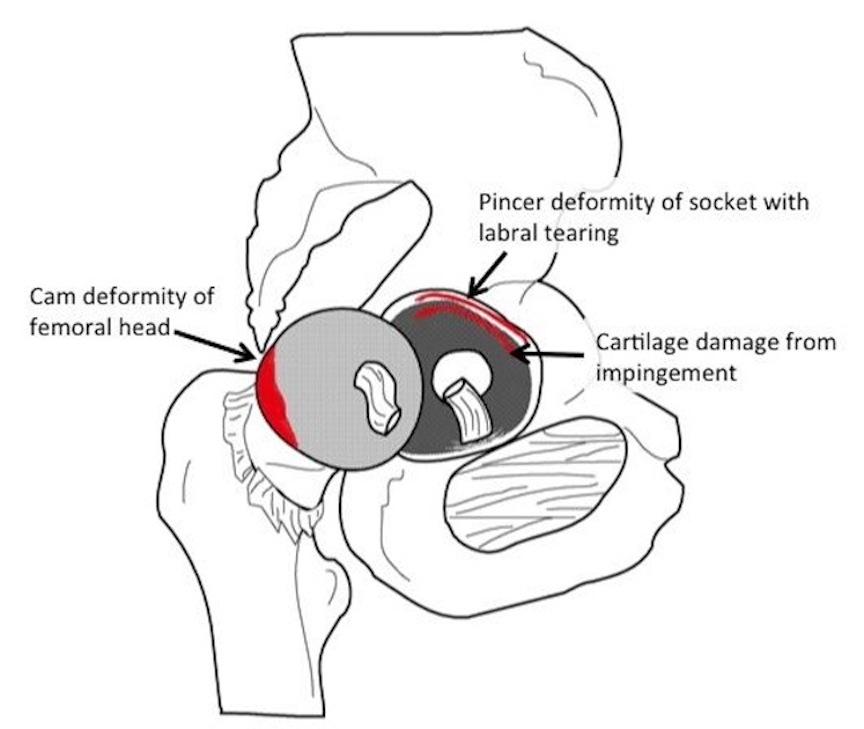
The majority of patients who undergo hip arthroscopy have an underlying diagnosis of femoroacetabular impingement (FAI). This is a structural abnormality of the hip joint, which may include a misshapen femoral head (cam impingement) or socket (pincer impingement) that causes pathological contact between the two bones during hip range of motion. These irregularities alter the biomechanics of the hip joint and pelvis and may result in labral and cartilage damage over time.
If a patient with FAI or traumatic hip injury is refractory to alternate means of pain relief – activity modification, physical therapy, steroid injections or medical management – surgery may be necessary to correct the underlying problem.
Accessing the Hip Joint
One of the challenges of hip arthroscopy has been gaining access to the joint. By utilizing a special table that can safely apply traction to the leg, adequate separation within the hip joint is possible, explains Gwathmey.
Once the patient is asleep and positioned, the ball or femoral head is pulled out of the socket approximately 10 mm to allow space for the arthroscope and other instrumentation for surgery. Only two to four 1-cm incisions in the side of the hip are necessary to perform the surgery, which means there is less blood loss and scarring than with open surgery.
Eliminating Pain at the Source
Once the camera is in place, it’s possible to identify the source of the problem and then take steps to correct the abnormality. “This may include reshaping the bone so that the ball and socket fit together better,” says Gwathmey. In addition, the surgeon may repair the damaged labrum or remove loose cartilage to address these mechanical sources of pain and dysfunction.
Ensuring Complete Recovery
Despite the minimally invasive nature of the procedure, major work is done within the joint. Patients undergoing hip arthroscopy will require four to six months of rehabilitation to regain motion, strength and balance. Gwathmey works closely with physical and occupational therapists to ensure patients have the resources they need to make a full recovery and return to the activities they enjoy.
“Rehabilitation is just as important as the surgery itself,” says Gwathmey. “Our therapists specialize in treating hip patients so they understand the nuances of hip anatomy and mechanics and play a critical role in reestablishing normal function for our patients.”
Watch the video to see a hip arthroscopy procedure performed on a male patient with labral and cartilage damage from FAI. This patient was an avid marathon runner until his hip pain progressed to the point that he could no longer run. His underlying hip abnormality combined with his strenuous activities caused significant damage to his hip joint.