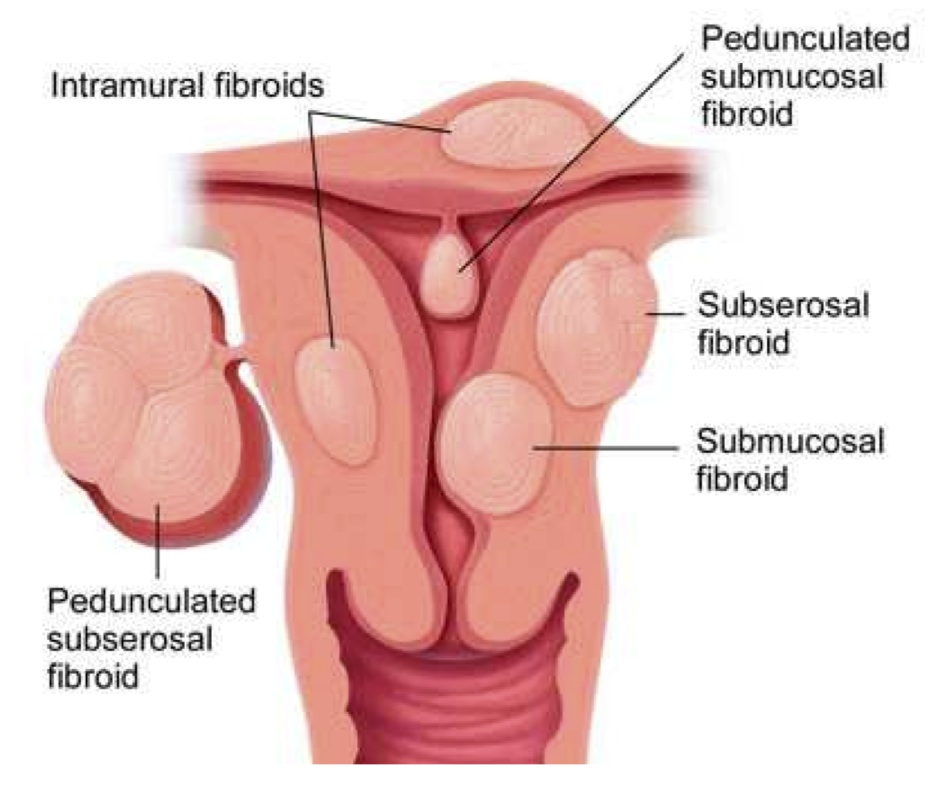
While not life-threatening, fibroids (benign growths that develop in the muscular wall of the uterus) affect the quality of life for as many as two out of three women in the U.S., according to Dana Redick, MD, Medical Director of the University of Virginia Uterine Fibroid Treatment Center. Symptoms are often misinterpreted or nonexistent, so this number may actually be even higher.
For those patients who experience the heavy bleeding, pain and discomfort of symptomatic fibroids, UVA offers the full range of treatment options through a dedicated Uterine Fibroid Treatment Center (UFTC), a unique collaboration among the departments of radiology and gynecology led by Redick and Alan Matsumoto, MD, Chair of the Department of Radiology and Medical Imaging. “The biggest advantage of having this multidisciplinary team is that we work together to educate patients on all of the varied treatment options available to them so that they may make an informed decision about which option would be best for their personal situation,” says Matsumoto.
Because UFTC is a multidisciplinary clinic, convenience is also a perk. Patients require fewer clinic visits and receive streamlined care in part because of the Center’s prescreening efforts. Before a patient arrives for her first appointment, physicians have an opportunity to review prior imaging or laboratories and discuss possible treatment options. Consults with gynecology, radiology or both are arranged as needed during that single visit. “[Radiology and gynecology specialists] now interact face to face in real time with patients to formulate as a team the best plan for treatment,” says Redick. “In one visit we accomplish what might have taken three visits before.”
In addition to the many standard treatment options available for uterine fibroids — medical therapy, endometrial ablation, uterine artery embolization, hysterectomy and myomectomy — UVA is pioneering advanced techniques that enhance recovery and limit recurrence.
It is one of the few centers in the country offering focused ultrasound treatment for uterine fibroids. And, with skilled surgeons like Redick leading the way, it is making complex procedures like robotic laparoscopic hysterectomy more widely available to patients. One patient’s experience with laparoscopic hysterectomy is highlighted in the case study below.
Case Study: Robotic Laparoscopic Hysterectomy
Patient: 41-year-old mother of three
Evaluated by: Dana Redick, MD, Medical Director of the University of Virginia Uterine Fibroid Treatment Center and Alan Matsumoto, MD, Chair of the Department of Radiology and Medical Imaging
Presented with: Pain and heavy vaginal bleeding
“The patient was seen by Dr. Michelle Rindos in the UVA Midlife Clinic in early January 2012,” says Redick. “Her vaginal bleeding was so heavy that she had an abnormal blood pressure and was sent to the emergency room. Her hemoglobin was at 9.8. She was then referred to me for treatment.”
Diagnosis: Uterine fibroids
Several uterine fibroids were pushing into the cavity of the uterus, causing severe bleeding. The largest measured 6.9 x 5.4 cm.
Recommended treatment: Laparoscopic robotic hysterectomy
“The patient and I discussed all of the available treatment options,” says Redick. “She wanted a hysterectomy, but couldn’t afford to take time away from work and her family. We opted to treat medically first with Lupron, followed by a laparoscopic robotic hysterectomy, which has a shorter recovery period than traditional hysterectomy. Prior to the procedure, Lupron Depot® effectively induced menopause, shrank the fibroids and reduced bleeding. It gave her time to improve her blood count and allowed her a three- to six-month window in which she could make arrangements for surgery.”
Procedure overview: Four small incisions, or ports, were made in the abdomen, ranging in size from 5–12 mm. Two of these ports provided access for the da Vinci® robot arms, which are fully wristed for easy maneuvering. A stereoscopic camera providing 3-D visualization was placed in the third port. The fourth was used to pass suction, suture and other laparoscopic instruments. Stationed at the surgical system console, Redick used finger and wrist controls to manipulate the robotic arms, successfully detaching the uterus. She then made an incision at the top of the vagina and slipped the uterus through this opening before suturing it closed. “The procedure took approximately three hours — a little longer than open surgery,” says Redick.
Outcome: The procedure was a success and the patient was discharged one day after surgery.
“I saw the patient 14 days after the procedure and she felt great,” says Redick. “She no longer required narcotic pain medications and was back to regular diet. She was sitting at her computer and doing work from home at that point, and she returned to the office within a few weeks of the surgery.”
Watch the video to hear more about this procedure from the patient’s perspective.
Learn more about the Uterine Fibroid Treatment Center.