At a Glance
- There are few satisfactory treatment options for infants born with irreparable mitral valves.
- UVA surgeons adapted technology used for blood vessel grafts in adult valve replacement to create a high-functioning valve for an infant.
- This case continues to inform future uses of the Melody® valve in young patients.
Congenital mitral valve disease in newborns is, fortunately, a rare condition. Because it is unique, however, advances in treatment are slow to develop. “There are very few options available for treating newborn infants with irreparable mitral valves, particularly when the annular size is less than 15 millimeters,” says UVA pediatric heart surgeon Mark Roeser, MD. “Traditional valves are too large, and the use of mechanical mitral valves is limited by the effect of anticoagulants on immature livers.”
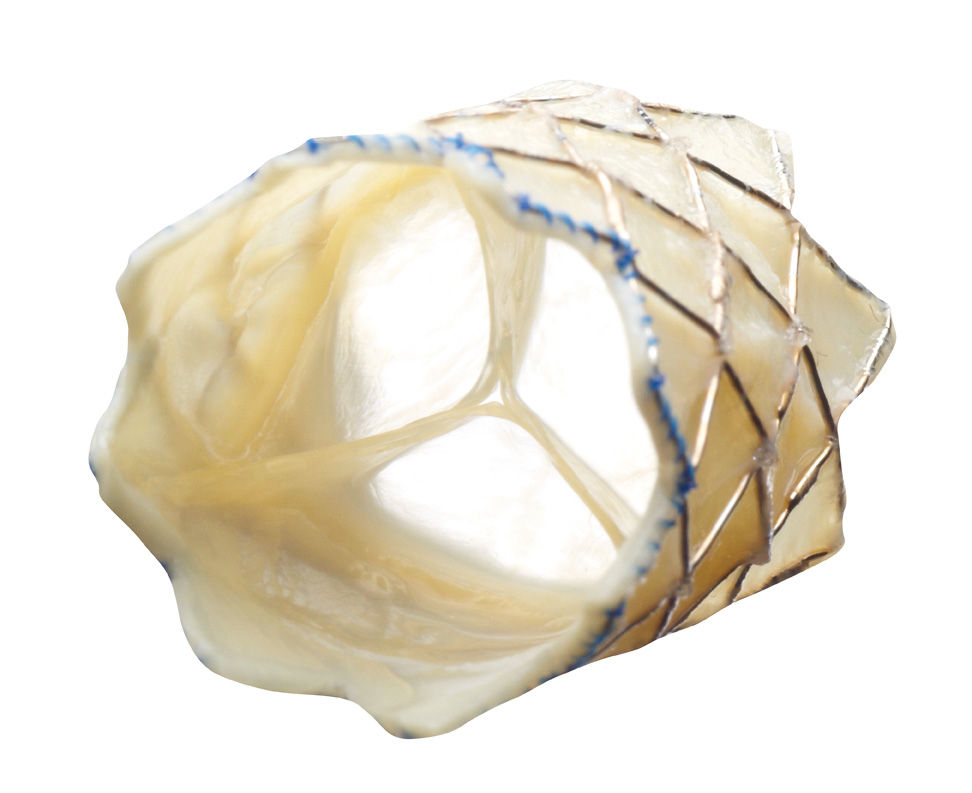
Over the last decade, surgeons have had success adapting the Melody® valve, a stented bovine jugular vein graft used in adults, for pediatric mitral valve replacement. Roeser estimates that there are approximately 12 centers around the country that have adapted the Melody valve for use in tiny patients. In fall 2018, UVA joined that group.
Roeser, his partner, surgeon Jay Gangemi, MD, and interventional pediatric cardiologist Michael Hainstock, MD, implanted a Melody valve in the smallest child reported so far, a 3.1-kilogram infant. “We are fortunate to have all the required expertise in fields like pediatric heart surgery, interventional pediatric cardiology and pediatric intensive care, to take on the challenge of an unusual case like this,” says Roeser.
Mitral Valve Replacement
Patient: Six-week-old infant
Presented with: Rapid breathing, jaundice, failure to gain weight, heart murmur
Evaluated by: UVA pediatric cardiology team
Diagnosis: Congenital mitral dysplasia caused by the lack of development of the posterior mitral valve leaflet
During the infant’s one-month exam, the family pediatrician detected a heart murmur and recommended that the parents consult with a local cardiologist. An echocardiogram demonstrated a mitral valve issue, and the local cardiologist referred the family to the UVA pediatric cardiology team, who made the final diagnosis.
Treatment: Valve implantation
The UVA team consulted with other cardiologists nationally, who confirmed their view that implanting the Melody valve was their best treatment alternative.
According to Roeser, the Melody valve offers a number of distinct advantages over other potential treatments. “We are able to modify the valve and the stent it is placed on in the OR and then sew it back together to fit even the smallest child. Then as the patient grows, the valve can be upsized with a balloon and ‘grow’ with the child,” Roeser says. “It also provides superior flow dynamics compared to a traditional valve, with no anticoagulation needed.”
Prior to the procedure, Roeser modified the Melody valve to facilitate surgical implantation (see video below). He added a sewing cuff around its midsection, shortened the valve and cut out a sinus wall so that the valve would not obstruct the left ventricular outflow tract.
melodyvideoshort from UVA Link on Vimeo.
Working collaboratively, the cardiac surgeon and a cardiac interventionalist compressed the Melody valve over a balloon catheter to allow passage through the mitral annulus, and sutured the valve in place. Once the valve was in position, the balloon was carefully expanded.
A small hole was then made to the atrial septum to allow access to the left atrium. This was done to facilitate subsequent percutaneous catheterizations, which will be needed to enlarge the valve to fit a growing child.
Immediate outcome: SVT controlled with beta blockers
The child went from having suprasystemmic right ventricular pressures to normal right heart pressures. His lung fields cleared rapidly and they did not reaccumulate fluid.
Due to the small size of the child, the conduction system was stretched during the procedure and he developed supraventricular tachycardia that was controlled with a beta blocker. Following a three-week recovery period, he was discharged from UVA, growing well and in a normal sinus rhythm.
Prognosis: Stable with future procedures to follow
The patient remains on beta blockers; he sees his local cardiologist in Lynchburg every two months for follow-up. Future procedures will be necessary to adapt the valve for his growing body.
“Our goal is to continue to expand the new valve as long as possible, helping us reach the point at which we can implant a valve more suited to a larger child,” Roeser said. “This will not only limit the number of open heart surgeries he has to experience over his lifetime, but will also reduce his stroke risk.”
In conjunction with the referring physicians, UVA will continue to monitor the child and enter outcomes data in a patient registry. “Every hospital in the United States that performs these procedures contributes to this database,” Roeser explains. “By looking at the data in aggregate, we can better understand the effectiveness of the procedure and make refinements to improve long-term outcomes.”