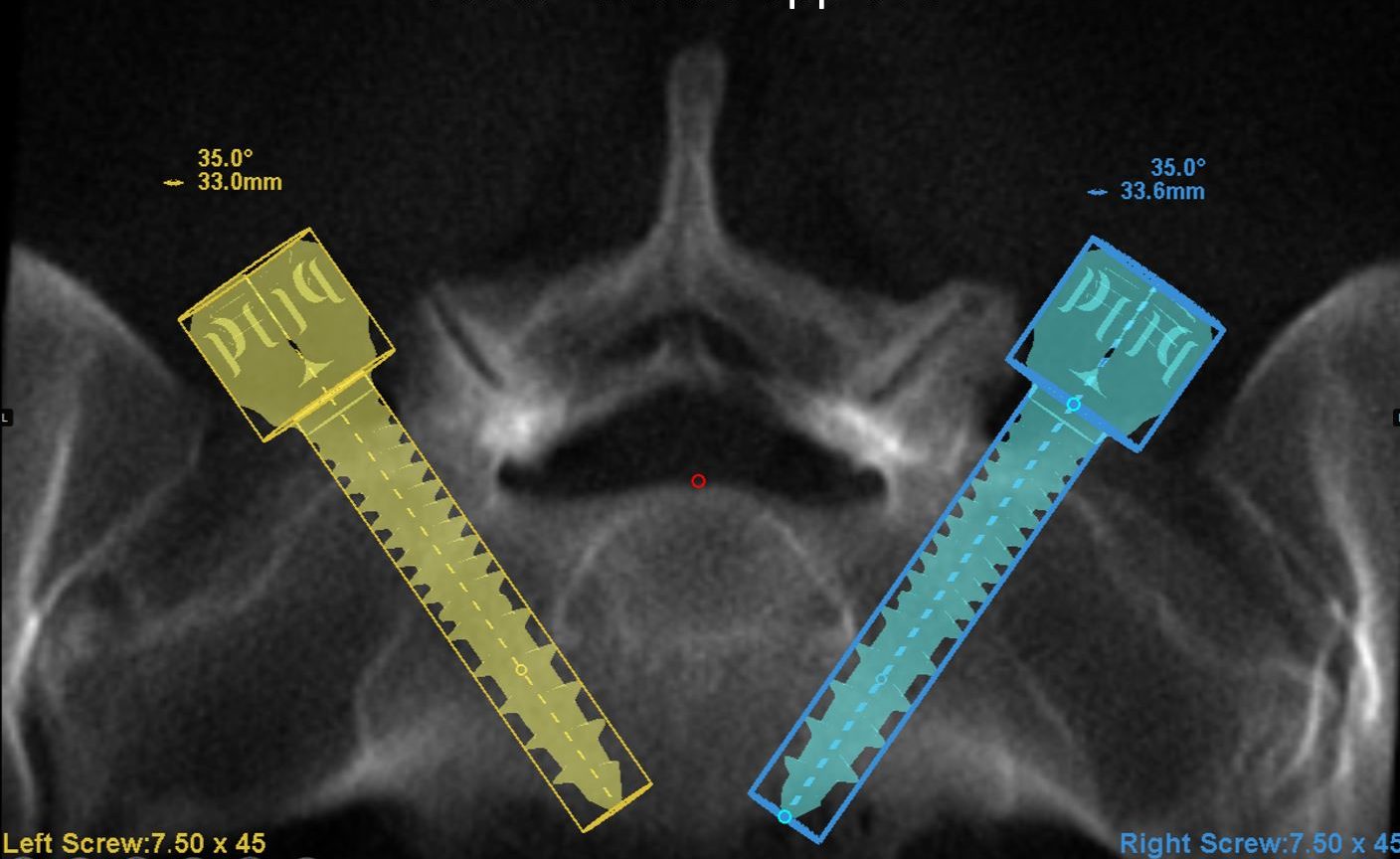
Spondylolisthesis is a spinal condition in which a vertebra slips over the vertebra directly below it. It is usually caused by degeneration or spondylolysis, a crack in one of the vertebra. Symptoms include lower back pain, buttocks pain and radiating pain in the legs.
Physical therapy to strengthen back and abdominal muscles and offload stress on the spine may be effective for some patients. However, for those who do not respond to nonoperative treatment, there is another option: the fusion of the slipped vertebra using screws and rods.
The procedure, says UVA orthopaedic surgeon Xudong Joshua Li, MD, PhD, is a complicated one. “According to literature reports, the width of L5 pedicle is slightly narrower, the height is shorter and the angle of the pedicle is wider in patients with spondylolysis than in patients without spondylolysis,” explains Li. “Thus, pedicle screw fixation in spondylolytic spondylolisthesis sometimes is challenging because of different anatomical characteristics of the pedicle. The spondylolytic spondylolisthesis fusion surgery requires a longer incision and increased surgical time, and risks include more blood loss, radiation exposure and more chances of infection. In addition, because of the limitations of the size of the incision, surgeons tend to insert screws with limited convergence.”
Robotic surgery, now widely utilized across many surgical subspecialties, has emerged as a solution to place pedicle screws accurately and minimally invasively. The benefits, says Li, include: decreased radiation exposure to both patients and the operating team, lower complication rates, shorter operative time and recovery time.
Case Study: Robotic Spine Surgery for Spondylolisthesis
Patient: 46-year-old female
Assessed by: Orthopaedic surgeon Xudong Joshua Li, MD, PhD
Diagnosis: L5/S1 Spondylolytic Spondylolisthesis
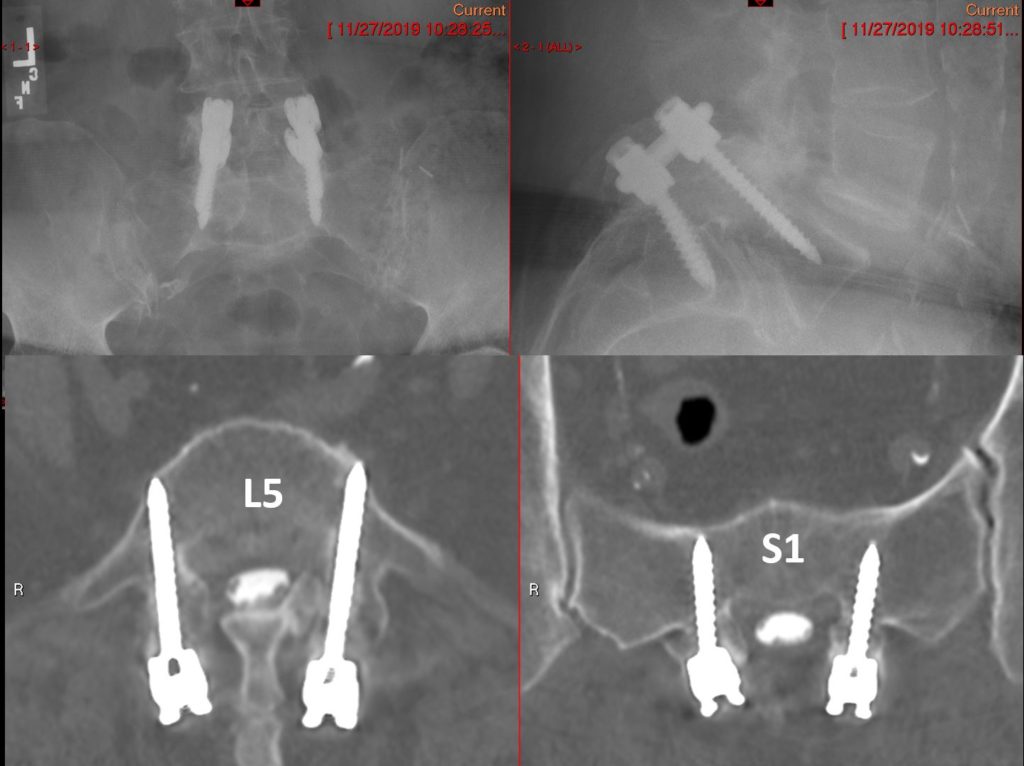
Figure above shows a patient with spondylolytic spondylolisthesis who had traditional surgery 15 years ago. This shows the screw placement in a divergent position that has unfavorable biomechanical property compared with a convergent position. An accurate screw placement is a prerequisite to achieve a successful reduction of the slip.
Treatment: L5/S1 transforaminal interbody fusion and posterior spine instrumentation fusion with robotic assistance
“Before surgery, we obtained a CT scan of the patient’s lumbar spine,” says Li. “These images were loaded into a computerized 3D planning system, which allowed us to make a detailed plan for the pedicle screw placement that took into account the screw diameter, length and trajectory angle. This was planned out before the patient entered the operating room, so every surgical team member knew the blueprint before the surgery.”
To prepare for the surgery, the robot was attached to the operative bed. The team placed a reference frame on the patient and postioned the robot. The surgeon then directed the robot arm to the planned pedicle screw insertion site, made small incisions and placed screws with the guidance of the robotic arm. “We still do the physical work of the surgery,” says Li. “But without the robot to guide us, we would have had to make a longer incision and perform excessive muscle dissection to achieve the large convergence required to prevent slippage of the vertebrae.”
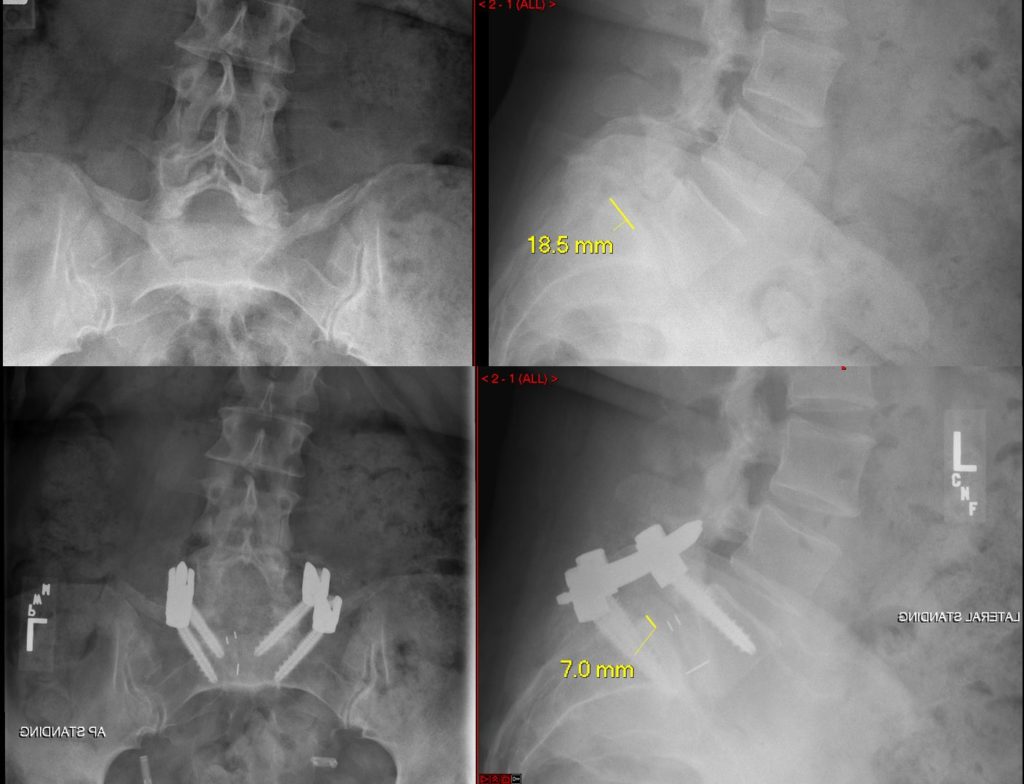
These scans above were taken before (upper panel) and after (bottom panel) the surgery, and show the placement of the screws with a larger convergence to ensure stability.
Recovery: Six weeks to full recovery
The patient remained in the hospital for 2 days. During this time, she had physical therapy to improve mobility. The incision healed in approximately 3 weeks, with full recovery achieved in around 6 weeks.
Outcome: Immediate pain relief and improved numbness
“The pain she experienced in both of her legs was relieved immediately after surgery,” says Li. “The numbness is remarkably improved and 90% of her lower back pain was gone within 6 weeks of the surgery.”
UVA Health is now open for in-person care for new and existing patients. Call UVA Physician Direct at 800.552.3723 to refer a patient.
To transfer a patient to UVA Health, call the UVA Transfer Center at 844.XFERUVA (933.7882).
Contact Us
Our Physician Relations Manager, Liz Nottingham, is available by phone (434.981.1023) or email to answer your questions and help with problem solving. Feel free to reach out to her as needed.