UVA welcomes one pediatric oncology fellow per year. Katye Herring, MD, is in her second year of this three-year program. Working alongside UVA Children’s oncologists William Petersen, MD, and Michael Engel, MD, she has been exposed to unique pathologies and complications, developed treatment plans for complex cases and cared for patients through every stage of disease, from diagnosis to recovery. “To have the ability to learn about each individual case that comes in is a great advantage for me,” she says.
The inclusion of residents and fellows in patient care benefits more than just the student, however. According to Petersen, the rich learning environment within a teaching hospital like UVA is a catalyst for better, more advanced and more hands-on care.
“Being involved in medical education and training makes everyone better,” he says. “When learning is happening all around you, it stimulates learning for every team member, from the least experienced to the most experienced. This helps ensure that everything we’re doing is up to date and cutting edge, and that we are providing the best possible care for our patients.”
Profiled in the case study below is one patient who benefitted from this team approach to care. “This patient received outstanding care from Dr. Herring from a medical standpoint,” says Petersen. “Dr. Herring also provided psychosocial support and worked with multiple pediatric subspecialists to offer the most holistic, comprehensive care possible for this family.”
“I think that, although these kids are going through something horrific, they want us to learn as much as we can so that we can care for future patients,” says Herring.
Case Study: Wilms’ Tumor
Patient: 2-year-old female
Primary Care Team: Pediatric oncologist William Petersen, MD, and pediatric oncology fellow Katye Herring, MD
Presented With: Distension of the abdomen with a painless lump on the left side
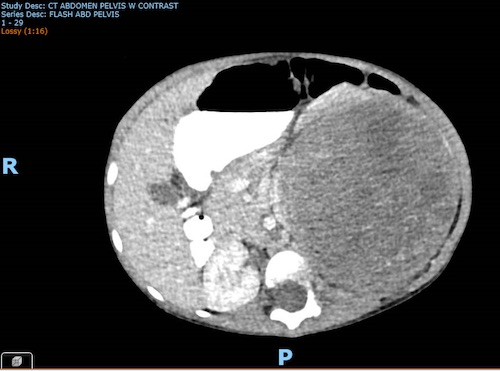
“Any time we have evidence of a mass, imaging is done,” says Petersen. “She had already had an X-ray and ultrasound prior to her arrival at UVA. We needed more detail, so we did advanced imaging, including a CT of the abdomen and chest.”
Diagnosis: Diffuse anaplastic Wilms’ tumor
The CT scan confirmed the presence of a tumor on the kidney, so the patient was admitted to UVA Children’s and scheduled for surgery. To pinpoint the exact type of tumor, surgeons opted to remove the entire kidney and the tumor rather than biopsy the mass. “In kids, the standard approach is to remove the entire tumor and the kidney because we know that if we cut into a malignant Wilms' tumor then the cancer cells can spill into the abdomen, which can make it harder to cure,” says Petersen.
The surgeon, Gene McGahren, MD, performed a resection of the left kidney and tumor, along with surrounding lymph nodes. The tumor was 10 cm x 10 cm x 13 cm. UVA pathologists evaluated the tumor and confirmed a diagnosis of diffuse anaplastic Wilms’ tumor (DAWT).
Wilms’ tumor is the most common type of kidney cancer in children; however, it is a rare diagnosis with approximately 500 cases per year in the U.S. “Diffuse anaplastic Wilms’ tumor is a more aggressive subtype of the disease and requires more intensive therapy,” says Petersen.
Treatment: 6 fractions of sedated radiation followed by 10 cycles of chemotherapy
Post-surgery, the patient remained in the hospital for one week to recover and heal. During that time, the pediatric oncology team met and discussed the most effective treatment options available for this specific diagnosis. “Once we decide on a recommended plan ourselves, we sit down with the family over many hours to discuss the treatment plan. We talk about every drug and every possible side effect so that parents are truly informed before giving consent,” says Petersen.
The patient received six fractions of sedated radiation and began her first course of chemotherapy in late August 2019. She was admitted to the hospital about once every three weeks for treatment and received a variety of drug combinations including: carboplatin, cyclophosphamide, doxorubicin, etoposide and vincristine.
The patient was administered additional medication to combat the side effects of treatment, including nausea and constipation. Her care team carefully monitored her kidney function and made sure her overall status was appropriate prior to beginning each new course of therapy.
“She was admitted to the hospital for three to five days every three weeks for seven months of treatment,” says Herring. “I’m really impressed with how she did. She was feisty and determined. If you came to look for her, she would be in the play room or wandering the halls. She loved the elevators and visits to the cafeteria.”
The patient had a few readmissions during the course of therapy due to fever and low neutrophil counts, according to Petersen. These are the white blood cells that help fight off bacterial infection.
Outcome: Cancer is in remission
The patient tolerated therapy surprisingly well, according to Petersen. She had an excellent response to treatment and did not have any disease on follow-up imaging as recently as two months ago. She is now six months removed from the end of her therapy and continues to be in remission.
“We won’t be able to say she is cured until five years out from treatment. However, it is good for us to celebrate the end of this journey and mark the end of treatment as a milestone,” says Petersen. “As we celebrate this, we have to be mindful that this is still a very serious diagnosis and a serious disease that can come back.” That’s why follow-up is so important.
Follow-Up: Scans every three to six months for five years, followed by survivorship care
The patient will return to UVA every three to six months for five years for a clinical exam and imaging tests to rule out recurrence. After she reaches the five-year mark, she will be transitioned to the UVA Pediatric Oncology Survivorship Clinic to monitor for the long-term side effects of cancer treatment.
Comprehensive and Family-Centered Care
This family had access to a variety of resources to help ensure their child was able to receive the care she needed in a supportive environment. Like many who rely on UVA for their care, this patient lived outside of Charlottesville and the commute was too great to bear during treatment.
UVA social workers were able to arrange housing through the Yellow Door Foundation, which provided a convenient place for the family to stay during treatment. “This was a lifesaver for this family,” says Herring. “It allowed them to be together as much as possible, which was good for [the patient]. It gave her a sense of comfort.”
To refer a patient to UVA Children’s Hospital, call UVA Physician Direct at 800.552.3723