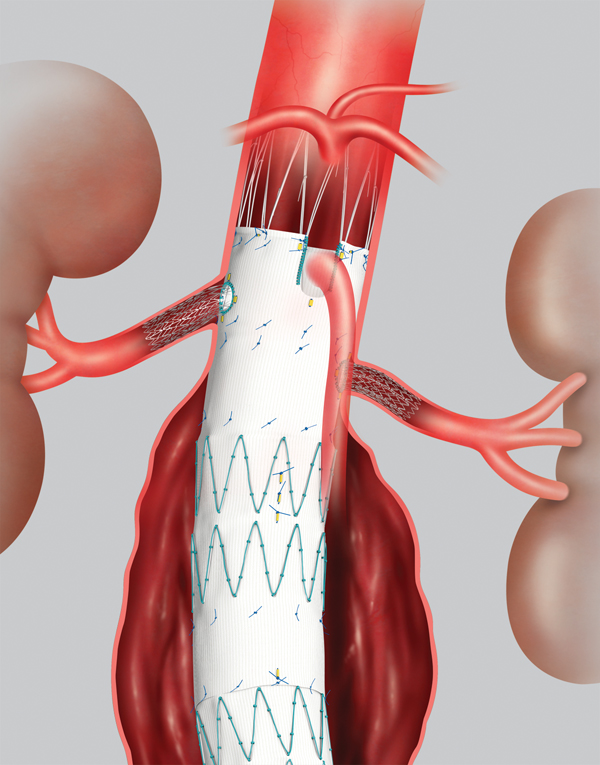
Endovascular repair is now the preferred method of treatment for approximately 75 percent of patients with abdominal aortic aneurysms. With the introduction of a custom fenestrated endograft, even those patients with pararenal aortic aneurysms (adjacent to the kidney arteries) are now candidates for this minimally invasive approach.
“Before we could only treat if the aneurysm was 1.5 cm removed from the kidney arteries,” explains Gilbert Upchurch Jr., MD, Division Chief, Vascular and Endovascular Surgery at University of Virginia Health System. “With this device, holes within the graft account for the two kidney arteries and, thus, allow us to preserve kidney function in those with a short infrarenal aortic neck.”
UVA is one of only a handful of centers in the region with the expertise necessary to perform the fenestrated endovascular graft procedure. “Technically, this procedure is very advanced so even though it is FDA approved, it has only been rolled out to a few centers in the region,” says Upchurch. “This is the next step in minimally invasive aneurysm repair for that 25 percent who were not candidates previously. Ultimately the entire aorta will be treatable with endovascular stents.”
Fenestrated Endograft
Device Overview
The device consists of an aortic cuff and a bifurcated graft, each constructed of woven polyester fabric sewn to self-expanding stainless steel stents. Each component comes in a range of lengths and diameters to accommodate varying anatomies.
Candidates
Qualifying patients include those with pararenal aortic aneurysm, an aneurysm close to the kidney arteries. Those who are not healthy enough to undergo open surgery may benefit from this minimally invasive endovascular approach.
Preparation
Careful preoperative imaging and measurement is required to ensure optimal device placement and functionality. Computed tomography and special 3-D angiography tools are used to determine the exact positioning of the renal arteries and the superior mesenteric artery (SMA). With these measurements, the stent can then be custom-made with the openings for the arteries in the appropriate place to preserve blood flow. The stent requires three to four weeks of development.
Procedure
As with most endovascular aortic aneurysm repairs, aortic access is gained through small incisions in the groin. The stent is then placed from the femoral artery to the aorta. The procedure typically takes three to four hours, and patients remain in the hospital for two days post-procedure.
Advantages
This minimally invasive technique offers the following benefits:
• Shorter recovery time
• Small incision that leaves little scarring
• Less blood loss
• Shorter hospital stay
Read more about the treatment options available at UVA for aneurysms.