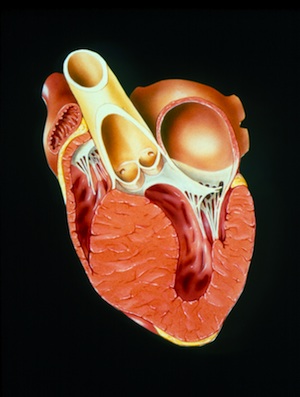
When an athlete collapses suddenly in midstride and dies, hypertrophic cardiomyopathy (HCM) is often the cause. It is tragic. It is unexpected. And it makes headlines. However, cases like these are not the norm. HCM is a genetic disease that causes an abnormal thickening of the heart muscle, which can lead to heart failure and sudden cardiac arrest. Yet what these occasional headlines obscure is the fact that tens of thousands of HCM patients are treated successfully for this condition and live normal lives.
The Hypertrophic Cardiomyopathy Association (HCMA), the leading patient advocacy group, wants to take HCM out of the news altogether by ensuring that all people with HCM receive the diagnosis and therapy they need. To do this, the HCMA is highlighting those centers in the U.S. that are offering comprehensive care for HCM patients. This year, it added UVA Health System to its list of 30 centers that have achieved accreditation as an HCM Center of Excellence, the only one in the state of Virginia.
“We were thrilled,” says Robert Battle, MD, the center’s co-director. “The HCMA board includes many of the field’s leading experts, and the review the organization conducts is extremely rigorous.” Battle believes that being named to this select group is a testament to the depth of UVA’s experience with HCM and the range of diagnostic, imaging, genetic and treatment resources it has to treat it.
A Pathway to Better Care
Although HCM is the most common inherited heart condition and the most common cause of sudden death in athletes, it is diagnosed rarely enough that the average cardiologist in general practice may see just one to two patients per year.
By creating centers, the HCMA helps direct patients to facilities with the expertise and resources to provide consistent, evidence-based care. Like other physicians at UVA, Battle has treated several HCM patients weekly for decades. This experience has given him a deep appreciation for the complexity of the disease and a nuanced approach to treating it.
“Phenotypically, HCM is a heterogeneous condition,” he says. “Some patients can be asymptomatic and live into their 90s, while others could have a profound phenotype that puts them at risk of sudden death early in life.” Battle and his colleagues approach every patient as an individual, working with them to maximize their ability to achieve their goals while respecting the constraints of their condition.
In developing a care plan for each patient, physicians at the center draw on a long list of specialists. Christopher Kramer, MD, Battle’s fellow co-director, lists the variety of specialists on staff at UVA with expertise in HCM. They include clinical cardiologists, interventional cardiologists and cardiac surgeons, as well as electrophysiologists, genetic counselors, psychologists and nutritionists. “It takes a multidisciplinary group of specialists,” Kramer says. “Being able to call on these specialists as we need them is an advantage of housing the [HCM Center of Excellence] within the Medical Center, rather than in a stand-alone facility.”
Genetic Testing for Earlier Diagnosis
In establishing the HCM Centers of Excellence, the HCMA also aims to identify more people at risk for the disease and offer them genetic testing. According to genetic counselor Matthew Thomas, ScM, one in 500 people are traditionally thought to have HCM, but more recent genetic and imaging studies suggest that the number may be as high as three in 500. “Genetic testing is one way we confirm or rule out a diagnosis,” Thomas says. “If the results are positive, we reach out to family members and encourage them to come in for testing.”
HCM is an autosomal dominant condition, which means that 50 percent of the offspring of people with HCM will also have the condition. Family screening is particularly vital in cases in which HCM is asymptomatic. “When you treat a patient with HCM,” Battle says, “you inherit an entire family of patients.”
A More Accurate Prognosis
A final reason for the HCMA to create centers of excellence is to increase the flow of patients participating in research studies and clinical trials. This makes particular sense in the case of UVA, which is one of 42 sites participating in a groundbreaking international research project to identify indicators that can be used to better predict the prognosis of the disease. Kramer is the co-principal investigator of the study, which the National Institutes of Health is funding with a $14.4 million grant.
Each of the 2,750 patients enrolled in the study undergoes comprehensive genetic and blood tests as well as cardiac magnetic resonance imaging using sophisticated techniques to measure heart muscle fibrosis. The investigators are tracking patient outcomes to determine if they correlate with genetic patterns, substances in their blood, or specific forms or quantities of fibrosis.
“If you have a more accurate way of predicting the course of HCM, you can be proactive in your choice of existing therapies,” Kramer says. “Being able to differentiate among specific HCM patients will also be useful in testing new approaches for the disease.”
Today, UVA physicians can offer patients therapies that can temper symptoms but cannot change the underlying pathology of the disease. “Being part of this study as well as an HCMA Center of Excellence makes UVA a logical place for patients to turn to for new approaches to diagnosis and treatment,” Kramer adds.
Learn more about the resources available to HCM patients at UVA.