At a Glance
- Stereotactic radiosurgery (SRS) is increasingly considered one of the more promising treatments for especially challenging brain tumors.
- The mainstay of SRS at UVA is the Gamma Knife®. UVA was one of the first medical centers in the world to adopt the technology almost 30 years ago.
- Whichever treatment is deemed most appropriate — SRS, resection, laser treatment, chemotherapy — the UVA approach to neuroscience and cancer care is collaboration across disciplines.
The complexity of brain cancer and the ever-growing number of options available to treat it means that optimal care requires collaboration. This is why UVA Cancer Center has assembled a multidisciplinary team of experts skilled in a variety of advanced treatment modalities.
“Cancer is a complex disease state that requires a comprehensive and cohesive treatment plan that is tailored to the individual patient,” says UVA neurosurgeon Jason Sheehan, MD, PhD. “We have the depth of experience, the range of world-renowned specialists and the broad portfolio of treatments to develop and pursue the optimal strategy for each patient that we see.”
In a specialty in which pinpoint accuracy, judgment and timing are paramount, stereotactic radiosurgery (SRS) is increasingly considered one of the more promising treatments for especially challenging tumors. Specialists at UVA are leading the charge to ensure this technology is used to its full advantage and to benefit patients worldwide. To do so, they go beyond providing the highest standards of care. In many cases, they have re-defined them.
Sheehan, for instance, is co-director of a first-of-its-kind patient registry established to improve clinical outcomes and cost effectiveness in SRS. Launched in partnership with the American Association of Neurological Surgeons (AANS) and the American Society for Radiation Oncology (ASTRO), the patient registry collects data from thousands of patients at 30 highly experienced radiosurgery sites throughout the United States — including UVA — in an effort to define patterns of care and establish benchmarks that will help advance the quality of care provided at leading academic medical centers as well as smaller community hospitals.
In addition, members of the team hold offices in national professional societies, teach practical courses to help community physicians learn or stay up to date with radiosurgery, edit peer-reviewed journals and write textbooks that shape the field. They are in an excellent position to bring the latest developments in SRS technology to patient care.
Gamma Knife and Beyond
The mainstay of SRS at UVA is the Gamma Knife®. UVA was one of the first medical centers in the world to adopt the technology almost 30 years ago. Since 1989, the UVA Gamma Knife team led by Sheehan has treated more than 9,000 patients from 55 countries and every state in the U.S.
“It is important to stress that the Gamma Knife is a brain-dedicated platform,” Sheehan says. “When it comes to brain surgery, no tool can be too refined and no team can be too experienced.”
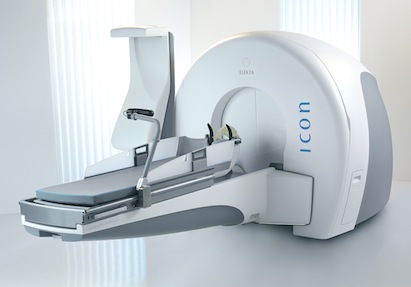
In 2016, UVA acquired the latest Gamma Knife technology, the Gamma Knife® Icon™, which has an accuracy of 0.15 millimeters, along with an integrated stereotactic Cone Beam CT and infrared tracking to provide real-time treatment plan correction in case of patient movement. Thanks to its unique targeting system and 192 high-energy Gamma ray fixed beams, the dose delivered to normal brain tissue is typically two to four times lower than with other technologies. The extracranial dose is 10 to 130 times lower than on other radiation devices more commonly used to treat cancers in the body and occasionally modified to treat brain tumors. This means that all patients, including children, can undergo a Gamma Knife procedure without detrimental effects on their overall health, performance and development.
The Gamma Knife is not the only SRS technology at UVA, however. As the situation demands, UVA also uses a variety of other technologies to treat brain disease. “We are not wedded to a single technology,” Sheehan says. “In many case, we conduct simulations on multiple platforms to determine which one is best for a particular patient.”
Whichever treatment is deemed most appropriate — SRS, resection, laser treatment, chemotherapy — the cornerstone of the UVA approach to neuroscience and cancer care is collaboration across disciplines. UVA will assemble a team to attack cancer on multiple fronts. “With a broad array of tools to treat brain cancer and an expert team to choose the right approach at UVA, chances for a successful treatment are dramatically improved,” Sheehan says.
To refer a patient to UVA Cancer Center, call UVA Physician Direct at 1.844.XFERUVA or 1.844.933.7882.