Patients with atrial fibrillation (AF) are more susceptible to blood clots and are five times more likely to experience a stroke, according to the Framingham Heart Study. To mitigate this risk, physicians typically prescribe oral anticoagulants or blood thinners like warfarin. However, not all patients are eligible to take this medication due to conditions that put them at high risk for bleeding, such as prior gastrointestinal bleeding, previous aneurysm or intracranial bleeding.
Finding a viable alternative to prevent blood clots in these patients has been the focus of multiple clinical studies over the past decade. In the course of this research, it’s been shown that more than 90 percent of blood clots form in the top left part of the heart called the left atrial appendage (LAA). This is where the blood tends to pool when the atria doesn’t contract, which is typical of AF. The stagnated blood forms clots, which can embolize and result in stroke. Occluding the LAA has shown promising results in reducing blood clots and, thus, lowering stroke risk in AF patients.
University of Virginia Health System is one of the only sites in Virginia currently offering three minimally invasive surgical options to occlude the LAA, giving patients choices where formerly there were few. “Some patients are better candidates for one procedure over the other, so we present all options and work with the patient to determine which is the best fit,” says UVA electrophysiologist Michael Mangrum, MD.
The options currently available at UVA include a newly adopted procedure using the Lariat™ suture device, as well as the existing Watchman® and AtriClip® devices.
Lariat
Approved by the Food and Drug Administration for the occlusion of soft tissue, the Lariat was utilized at UVA for the first time this summer. To determine if patients are candidates for this device, a comprehensive evaluation is performed, including a CT scan of the heart. “If the appendage is too big or if it’s angled the wrong way, then patients are excluded,” explains Mangrum. “Approximately 10 to 15 percent of patients are excluded after the CT.” Patients who have had prior heart surgery are also excluded.
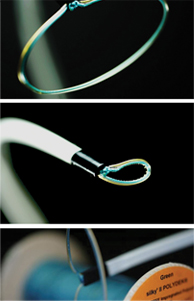
During the procedure, a catheter is placed in the left atrium via the femoral vein and another is placed in the pericardial sack, accessed via a puncture under the sternum. Magnetic guide wires are then threaded into position with fluoroscopic guidance to facilitate the placement of a pretied, braided polyester suture loop. Once placed over the LAA, the loop is then closed, and an echocardiogram confirms that the LAA is effectively occluded prior to removing the guide wires. The procedure lasts approximately two hours, and patients require one overnight stay in the critical care unit.
UVA is the first to offer this procedure in central Virginia. According to Mangrum, it requires an entire team of trained specialists – anesthesiologists, echocardiologists, electrophysiologists as well as a backup surgeon – to ensure success. “Moving the catheter in the left atrium and through a pericardial access can be challenging,” says Mangrum. “We underwent extensive training that included proctoring from other experienced operators.”
AtriClip
The AtriClip is a clip-like device that was approved by the FDA in 2010 for LAA occlusion. While the device is still implanted via open surgery in some patients at UVA, cardiovascular surgeon Gorav Ailawadi, MD, says there is now a minimally invasive option that is proving just as effective in those patients who have not had prior heart surgeries.
“We have implanted more than 50 of the AtriClip devices using a small-incision technique,” says Ailawadi. “There is no need to break ribs; we just need two 5 mm incisions – one for a scope, another for a retractor; and one 2 cm incision for the device.” After the device is clamped over the LAA, a transesophogeal echocardiogram ensures the device is placed correctly and occludes the entire appendage. Recovery is typically no longer than two days.
Ailawadi adds that the AtriClip is gentler than some devices, which is important because the LAA is a fragile part of the heart that is easily damaged. The risk for tearing or future bleeding is low with the AtriClip. While the device has a proven track record and FDA approval for occluding the LAA, Ailawadi says UVA is preparing to take part in a multicenter trial over the next year that would focus on proving its link to stroke prevention in AF patients.
Watchman
UVA has been an ongoing participant in the PREVAIL continued access protocol study, a registry that examines the safety of the implant procedure for the Watchman device. The results of the study have not been published, according to UVA cardiologist Rohit Malhotra, MD, so the device has not yet been approved for stroke prevention by the FDA. The original study (PROTECT AF) demonstrated that the device was equivalent to warfarin for stroke prevention. UVA continues to offer this procedure to a limited number of patients through clinical trial.
Unlike the Lariat and AtriClip, which occlude the LAA by restricting bloodflow using external devices, the Watchman is inserted inside of the heart, at the opening to the LAA. A catheter-based procedure, it involves accessing the left atrium percutaneously through the femoral vein. Once the appropriately sized device – there are five sizes – is deployed into place, a transesophogeal echocardiogram ensures proper positioning and that there are no leaks. The procedure lasts approximately two hours and the patient is kept overnight for monitoring.
For up to 45 days after the procedure, patients are required to take blood thinners, which excludes those who have absolute contraindications for these drugs. However, once that period is up, blood thinners are no longer needed.
The occlusion of the LAA using these minimally invasive techniques limits the risk for infection, decreases blood loss and shortens recovery time. UVA offers three different approaches to address the needs of more patients. “In most patients with AF, their stroke risk is not addressed,” says Mangrum. “They should be on blood thinners if possible, but if that’s not an option, we have a variety of effective minimally invasive solutions.”
To determine if your AF patient is at an increased risk for bleeding, calculate his or her HAS-BLED score.
Use the CHA2DS2-VASc calculator to determine your patient’s stroke risk.