Before transoral robotic surgery (TORS) was available, some patients with cancers of the tonsils, tongue base and supraglottic larynx chose to undergo radiation and chemotherapy rather than face the rigors of surgery — even when surgery offered the possibility of avoiding the long-term side effects of chemotherapy and radiation regimens. That’s because traditional open surgery often required surgeons to split the jawbone in order to reach the tumor.
Thanks to TORS, many of these patients no longer have to make this choice. Approved by the FDA in 2009, TORS allows surgeons to operate through the mouth. This means no visible scarring or disfigurement, fewer complications, shorter hospital stays and faster recovery. The UVA Department of Otolaryngology has been offering TORS since 2010. Mark Jameson, MD, PhD, and David Shonka Jr., MD, are two of the surgeons that offer this procedure. “For patients for whom surgery is recommended, this is a major advance,” says Shonka.
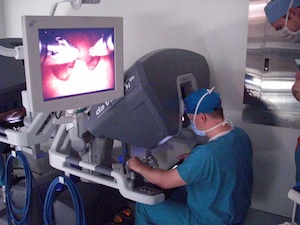
During TORS, surgeons use three of the four arms on the da Vinci® Surgical System — two to manipulate specially designed instruments and a third to aim a telescope with two high-performance cameras. One surgeon sits at a console, watches a detailed 3-D image on a screen and manipulates the robotic arms, while the other is stationed next to the patient.
Although it represents a high-tech departure from traditional approaches, the robotic system has been carefully designed to build on endoscopic and microscopic techniques that surgeons have already mastered. “The beauty of this approach,” says Jameson, “is that the image is so good and the robotic hands mimic us so well that there wasn’t a great deal of adaptation required on our part. The big difference is that the robot’s hands are a lot smaller than ours and can get to places where we couldn’t.”
Although Jameson and Shonka have used TORS for patients in their 80s, it is particularly beneficial for younger patients with small- to moderate-sized tumors who are reasonably healthy and who would benefit from being spared the long-term effects of radiation or chemotherapy. But both surgeons emphasize that TORS may not be appropriate for all patients. “Our goal at UVA is to offer the best treatment option for a person’s particular tumor,” Shonka says. ”This can mean surgery, radiation or chemotherapy, individually or in combination.”
Case Study: Transoral Robotic Surgery
Patient: Allen Lecco, age 56
Presented with: No symptoms. A neck mass was identified during a follow-up examination by his primary doctor for a serious neck injury incurred 35 years earlier.
Evaluated by: Head and neck surgeon David Shonka Jr., MD.
Diagnosis: Lecco had a growth on his tonsil and a growth in a lymph node on the same side of his neck. He was diagnosed with Stage 3 oropharyngeal squamous cell carcinoma.
Treatment Plan: Given the clinical staging of his cancer, UVA physicians gave Lecco the option of getting radiation with chemotherapy or having surgery. “He was a good candidate for robotic surgery,” Shonka says. “He had a mobile tonsil mass, which meant that there was a high likelihood that we could perform a transoral resection and remove the tumor with clear margins. In addition, the single lymph node on his neck didn’t look like it had any extracapsular spread and was very well contained.” Lecco elected to have surgery.
Procedure: After anesthetizing Lecco, Jameson and Shonka intubated him with a small endotracheal tube and positioned a retractor in his mouth to expose the tonsil and the back of the tongue. Once they had a good view of the cancer and secured the endotracheal tube, they moved the robot into position. Jameson sat at the bedside and assisted with positioning the retractor and robotic arms. He used two suctioning devices to ensure good visibility while Shonka operated the robot to remove the cancer. They then sent frozen-section margins, which were all clear. The surgery team did not perform a closure because the surgical defect was small enough to heal on its own. Lecco was released the next day.
Two weeks later, Lecco returned to have the lymph nodes in his neck removed. All the nodes were negative except the one node visualized during initial presentation. That node was reasonably small at three centimeters.
Outcome: “He responded well to both operations,” Shonka says. “We didn’t treat him with anything else after surgery. We’ve just been keeping an eye on him.”
Three years later, Lecco is cancer free and has nothing but praise for the care he received. “Everyone did an excellent job clearly explaining my options, describing the procedure and letting me know what to expect,” Lecco says. In fact, Lecco was so impressed that he recommended his uncle come to UVA when he developed a similar condition. He too underwent TORS with a good outcome.
Read more about treatments available for head and neck cancers at UVA Cancer Center.