The field of heart failure medicine has advanced tremendously over the past two decades. Medical therapies have improved and left ventricular assist devices (LVADs) have proven to be a durable solution for patients with end-stage heart failure. At University of Virginia Health System, we continue to advance our knowledge of heart failure through participation in national clinical trials. We are excited to announce two new trials for patients with heart failure.
A Next-Generation LVAD
As one of 60 centers participating in the MOMENTUM 3 Clinical Trial (IRB-HSR# 18090), the UVA heart failure team will evaluate the safety and efficacy of the latest generation of LVAD, the HeartMate 3™ device.“UVA has a long history with LVADs. We have been involved with this technology since its inception in the 1990s,” says John Kern, MD. “Because of our positive outcomes — which can be attributed to the level of expertise among our heart failure team — we have been asked to be a part of the approval process for this new technology.”
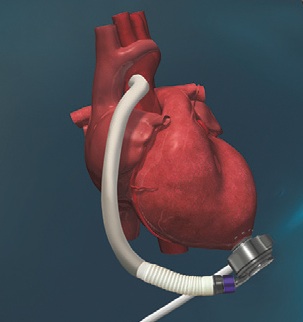
The HeartMate 3 is the first completely magnetically levitated device that lacks mechanical bearings. It has been designed with the goal of improved hemocompatibility, with large blood flow pathways to reduce blood trauma and minimize late thrombotic and bleeding complications. “Because of the potential for reduced complications for this new device, we are hopeful that physicians who have patients meeting the qualifications will refer them sooner,” says Kern.
Now enrolling, the MOMENTUM 3 study will evaluate the device as an alternative to the Heartmate II for use as long-term/destination therapy, as well as a bridge to transplantation. Compliant patients with any of the following indicators of worsening heart failure may potentially be eligible:
- Two or more heart failure admissions in the past year
- Inotrope requirement, either intermittent or continuous
- NYHA class III-IV symptoms
- Increasing diuretic requirement
- Decreasing tolerance of ACE/ARB and beta blocker
- Worsening renal function
- Pulmonary hypertension
- Hyponatremia
- Cardiac cachexia
- Lack of response to biventricular pacing
- Recurrent ventricular arrhythmia
Uncovering the Potential of Stem Cell Therapy
A small study involving just eight core sites in the U.S. and Canada, the Cardiothoracic Surgical Trials Network (CSTN) Stem Cell Trial (IRB-HSR# 17819) is a National Institutes of Health (NIH)-funded study evaluating the safety and efficacy of intramyocardial injection of allogenic mesenchymal stem cells, and the impact of these stem cells on myocardial function in LVAD recipients. The long-term goal is to determine whether stem cell therapy can augment ventricular recovery and prevent patients from requiring a heart transplant.
“This is a collaborative effort of cardiac surgery programs that provide excellent clinical care, have a high degree of expertise and answer real world questions to generate data that can improve the field as quickly as possible,” says Kern. “This will not take years to figure out.”
Patients participating in the study will receive an injection of stem cells into the left ventricle at the time of LVAD implantation. “We will follow these patients closely and rigorously after implantation,” says Kern. “There will be a weaning process that occurs in which we turn down the pump — this way we can infer whether the heart seems to be recovering function, which would mean that the stem cells are regenerating into viable heart muscle.”
Inclusion Criteria
To be eligible to participate in the CSTN Stem Cell Trial, adult patients should meet the following criteria:
- Scheduled to receive an FDA-approved LVAD for bridge-to-transplantation or destination therapy
- No history of cancer (excluding basal cell carcinoma)
- No MI or stroke within past 30 days
- No arrhythmia ablation planned at time of LVAD implantation
- No acute or chronic infectious disease, including HIV, or active systemic infection within 48 hours prior to randomization
Make a Referral
“UVA is an ideal choice for patients with end-stage heart failure because we have new clinical trials like these, in addition to standard treatment,” says Kern.
To refer a patient to one of these trials, please contact Nurse Coordinators Sandra Burks, Faith Mawyer or Rachel Simon at the Surgical Therapeutic Advancement Center office at 434.243.0315, or by email at uvastac@virginia.edu. You may also contact Principal Investigator John Kern, MD, at 434.982.4301.
To refer a patient for heart failure consultation or treatment, contact a UVA cardiologist by calling UVA Physician Direct at 800.552.3723 or reach out to our Referral Services team for assistance.