According to an article in ATS Journals, a publication of the American Thoracic Society, heart, kidney and liver transplants have a half-life of approximately 10 years; for lung transplants, that number drops to five. In an effort to improve the odds for patients requiring lung transplant, UVA Health System is utilizing new technology and transplant techniques to ensure donated lungs are of the highest quality and are the best match for the recipient. “This technology will help give patients better quality lungs and better matches, which we believe will improve life expectancy,” says UVA thoracic surgeon Mark Roeser, MD.
Introducing Ex Vivo Lung Perfusion
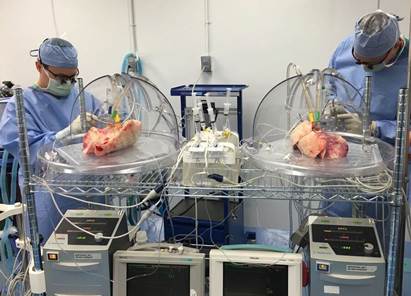
UVA is one of just over a dozen of hospitals nationwide now using ex vivo lung perfusion (EVLP). With a host of tubes that lead into a transparent domed chamber, the innovative device was initially developed in Sweden to assess the quality of harvested lungs. However, researchers in Toronto took the science a step further so that today, the device is used not only to test lungs, but also improve their function. In other words … it brings lungs back to life.
dozen of hospitals nationwide now using ex vivo lung perfusion (EVLP). With a host of tubes that lead into a transparent domed chamber, the innovative device was initially developed in Sweden to assess the quality of harvested lungs. However, researchers in Toronto took the science a step further so that today, the device is used not only to test lungs, but also improve their function. In other words … it brings lungs back to life.
Compared to the kidneys or liver, lungs are more difficult to harvest because they are more vulnerable to injury or infection. In fact, only around 1 in 5 lungs from deceased donors is viable for transplant. Toxins that flood the body at the time of brain death, as well as medications administered to organ donors to prolong the body’s natural state, can damage the lungs, as can the use of a ventilator, says Roeser, head of the EVLP Program at UVA.
EVLP allows physicians to remove the lungs and keep them in a controlled environment. “The lungs may actually be better than they appear in the body,” says Roeser. “Once we remove the lungs, we can connect them to the ex vivo circuit and inflate them slowly to see how they expand and contract outside of the donor body. We can also manipulate them to make sure they are functioning at the highest level prior to implant.”
The EVLP Circuit Explained
After lungs are removed from the donor, they are cooled prior to transport to slow metabolic activity. Upon arrival at the destination OR, they are attached to the EVLP circuit, which includes a pump and a ventilator. The pump infuses the lungs with a clear Steen Solution™, which allows for the warming and reperfusion of the lungs without a blood product, eliminating the risk of blood-borne pathogens or antibodies. The ventilator allows the lungs to respire.
Any existing blood is flushed from the lungs and excess fluid is eliminated to optimize lung function. “We can see the inside and outside of the lungs,” says Roeser. “We check the airway compliance, we check blood gasses and hemodynamics of the solution going through the lungs to make sure the lungs are adequate.”
Taking this process a step further, UVA is involved in a study funded by the National Institutes of Health to assess a drug that has been shown to reduce the risk for early graft dysfunction after transplant when used in tandem with EVLP. “The drug, called Reg, was developed at UVA for cardiac imaging, so it has been FDA approved for human use,” says Roeser. “We are hoping that this drug will prevent lungs from reperfusion injuries resulting from the influx of calcium that occurs when an organ goes from not having blood flow to suddenly getting blood flow. Our study should start early this summer.”
Expanding the Donor Pool
Typically, lungs are viable for six hours after harvesting from the donor. With EVLP, you’re essentially restarting the clock from the moment the lungs are connected to the circuit for reperfusion. “Now you may have 12 hours to harvest the lungs and prepare them for transplant rather than six,” says Roeser. “We could essentially fly from Charlottesville to California to get lungs if that’s where we found the best match.”
When it comes to finding the best match, lungs are assessed based on size, cross-matching antibodies and HLA (human leukocyte antigen) typing. Because of the time restrictions, the pool of available lungs has been limited to areas in close proximity to the list site; however, EVLP changes that. “With this technology, we’re moving closer to personalized lung transplants,” says Roeser. “Rather than looking for the best lungs in your area, in five to 10 years, we’ll be looking for the best lungs for you in the country.”
A History of Transplant Success
UVA Health System has been performing lung transplants since 1990 and now averages approximately 20 per year, with 10 successful transplants performed this year including a pediatric transplant. Its one-year survival rates for lung transplant are among the best in the country. “We typically have 95 to 100 percent survival every year, one-year post transplant,” says Roeser.
With the introduction of EVLP, UVA now has the opportunity to offer patients a broader selection of quality lungs. In addition, UVA’s transplant team is experienced in redo lung transplant procedures, which Roeser says will likely become more common.
“This will be important as more younger people require lung transplants,” says Roeser. “For example, we have medications now to keep cystic fibrosis patients alive longer, so they may require a transplant at age 30. Considering the average life expectancy with donated lungs, they would require another transplant at age 40 or so. Because the heart and other systems are typically in good shape at that age, another transplant would be entirely possible if you have a team experienced in redo transplant procedures.”
Learn more about the UVA Lung Transplant Program.
To arrange a meeting with a member of our lung transplant team, contact UVA Physician Relations.