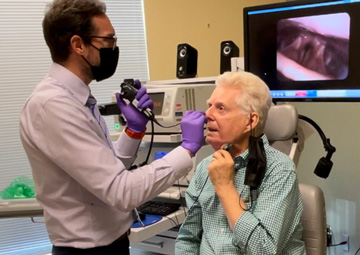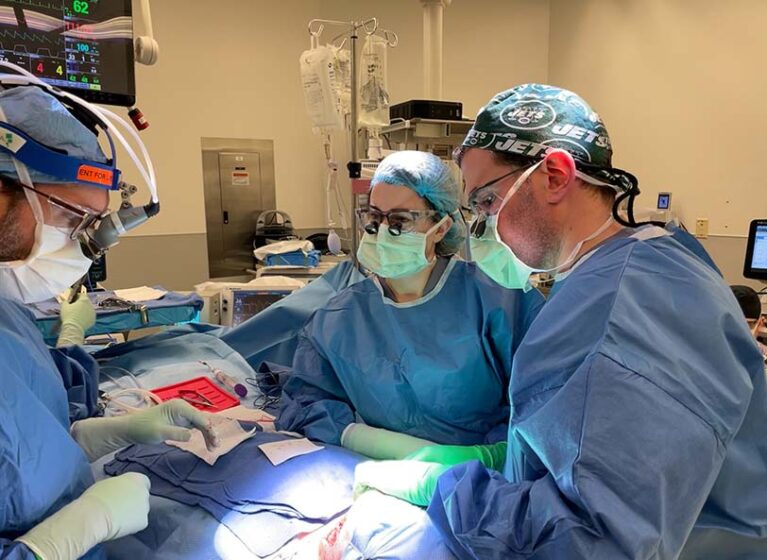
Selective laryngeal reinnervation, a novel procedure for correcting bilateral vocal fold paralysis (BVFP), is only practiced by approximately 20 surgeons worldwide. One of them is James J. Daniero, MD, who established the Division of Laryngology and Voice Care within the Department of Otolaryngology-Head and Neck Surgery at UVA Health.
Transposing Functional Nerve Restores Speech, Breathing & Swallowing
Traditional surgical treatments for vocal cord paralysis take a non-specific unilateral approach in which a nerve is transferred to the vocal cord without the intent for functional movement. While this approach allows static signals to pass into the vocal cord, it only maintains muscle bulk and forces the other side of the larynx to maintain all of the vocal cord function.
BVFP, one of the most severe complications of thyroid surgery, affects the bilateral recurrent laryngeal nerves in both sides of the larynx. Until now, there has not been an effective surgical treatment to correct this condition, which causes speech, breathing, and swallowing problems that weaken the voice and often result in a tracheotomy.
"Many physicians consider BVFP to be a permanent injury," Daniero says. "They are not aware of this novel surgical technique and its ability to achieve functional larynx rehabilitation because we're just starting the process of disseminating information about it."
'Holy Grail' of Larynx Function Nerve Restoration
In selective laryngeal reinnervation, surgeons transpose the phrenic (diaphragm breathing) nerve into the vocal cord muscle, creating new highways for information to be sent from the brain to the voice box. The transposed nerve sends respiratory signals from the brain through the diaphragm and to the posterior cricoarytenoid muscle that controls the vocal cords, telling the vocal cords to open and pull air into the lungs.
The procedure also involves borrowing a branch of the hypoglossal nerve and bringing it together with the remainder of the recurrent laryngeal nerve, allowing the vocal cords to close for speech.
As Daniero explains, selective reinnervation is the "holy grail" of larynx function nerve restoration because it removes the limitations of nonselective reinnervation, which only targets activation of one muscle. Instead, with selective reinnervation, abductor and/or adductor muscles are separately reinnervated for function-based reconstruction.
"Bilateral recurrent laryngeal nerves control multiple functions within the voice box," he says. "Reconstructing those nerves with traditional methods doesn't allow the nerve to know which function to activate, so it doesn't provide any function at all."
Learning at the Foot of the Originator
Daniero developed his skills in selective laryngeal reinnervation under the tutelage of the procedure's creator, Jean-Paul Marie, MD, PhD, of University Hospital in Rouen, France. He further refined those skills through careful collaboration with David Moyer in UVA Health's surgical anatomy lab. There, Daniero conducted complex nerve transfer surgeries, including 9 separate neurorrhaphies, on cadavers to identify the location of and access points for the nerves and to define how much distance needs to be traversed for reconstruction.
The handful of surgeons internationally who practice the technique, Daniero notes, collaborate regularly via text message to share ideas and develop best practices about this paradigm shift in treatment.
First Surgery Leads to Impactful Results
Daniero's first surgical case was a patient in their 20s who had both vocal cord nerves paralyzed after complications from thyroid surgery. A month after treatment, the patient was breathing better and starting to recover their voice.
Daniero credits a team approach for the successful result.
The procedure benefitted from his partnership with Jonathan Garneau, MD, a specialist in head and neck oncology and microvascular surgery. Together they worked to "re-wire" the neurologic input to the larynx by connecting several nerve grafts to nearby nerves through microsurgical techniques. An expert team of lead surgeons, resident physicians, and nursing staff contributed to the operation, managing the various components involved and ensuring a quality outcome.
Timing Amplifies Success
Patients under 50 years of age are the best candidates for the procedure, according to Daniero, because they have better neuroplasticity, which allows the brain to learn or construct new pathways for activating function in the voice box. He says the key to success is conducting the procedure within 18 months of injury.
"Patients need to be evaluated at the earliest possible stage for selective laryngeal reinnervation to be a potential solution," Daniero says. "The timeframe and age restrictions, coupled with the fact that many referring physicians aren't yet aware of this unique, advanced surgical technique means the current patient population is small. However, for those who have been treated, it has been quite impactful."