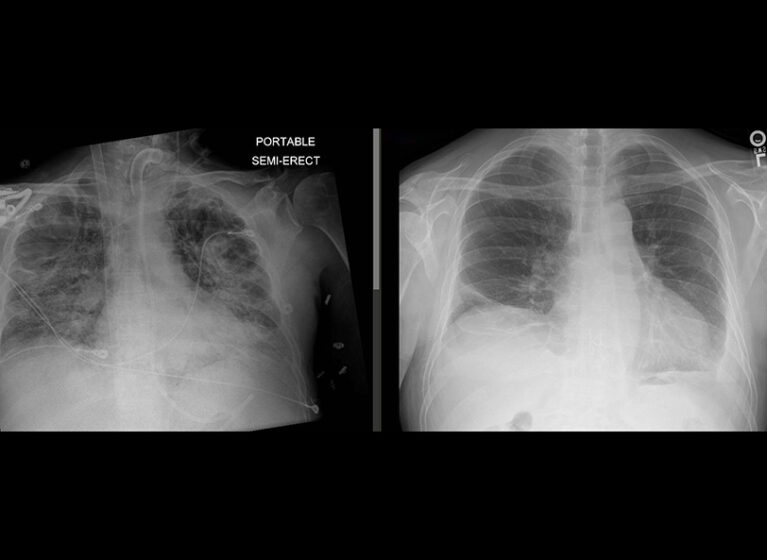
With COVID now a major indication for a lung transplant, the pandemic dramatically altered the pulmonology landscape.
The pressing issue? When to consider lung transplant for COVID-related lung disease (CRLD). UVA Health experts are leading the way to help answer that question.
“When someone is on respiratory life support — how long do you wait for them to recover before considering lung transplant? We have the same question in the outpatient setting with patients who develop post-COVID fibrosis,” says pulmonologist Hannah Mannem, MD, who serves as medical director for the UVA Health lung transplant program.
She’s an author of two recently published papers sharing expertise on COVID-related lung transplant, and her UVA Health colleague, Max Weder, MD, is the lead author of a Transplantation expert insight piece on the topic.
Specializing in interstitial lung disease and lung transplant, Mannem has the ideal perspective to bridge these two fields. She’s one of 6 subspecialists in UVA Health’s comprehensive Interstitial Lung Disease Program. The ILD Program is well known for leading the field’s groundbreaking PRECISIONS trial and is now at the forefront of understanding COVID’s long-term pulmonary impact.
Lung Transplant Shifts to Acute Setting
UVA Health was among the nation’s first centers to perform a COVID-related lung transplant and has done a handful more to date.
The noteworthiness of this transplant early in the pandemic, Mannem explains, results from the unusual consideration of “performing a lung transplant in an acute situation and with a patient on full life support. It was innovative and monumental for our field.”
Mannem is the second author of a Chest review in the journal’s "How I Do It" series. Published January 2022, the review offers guidance and 2 case studies on how to approach lung transplantation for post-COVID fibrosis and COVID-related acute respiratory distress syndrome (CARDS).
The authors note: “Transplant physicians must weigh the risks and benefits of lung transplantation differently in a post-COVID fibrosis patient who is likely to remain stable or gradually improve in comparison with a patient with a known progressive fibrosing interstitial lung disease.”
Because many COVID patients recover lung function, Mannem notes, the data suggest waiting 4-6 weeks for CARDS and 3-6 months for post-COVID lung fibrosis before referring to transplant.
Advocating for Global Lung Transplant Registry for COVID
Mannem’s colleague, Weder, is lead author of an expert insight piece in Transplantation. Published in January, the review provides clinical expertise on lung transplants for CRLD and notes how COVID became the nation’s 3rd leading indication for lung transplant in 2021.
COVID-Related Lung Transplant By the Numbers
Source: Transplantation, January 2023
In 2021, COVID accounted for almost 10% of the entire U.S. lung transplant volume.
Since Oct. 2020, COVID led to 364 lung transplants. Of those:
223 for COVID–related ARDS
141 for COVID–related fibrosis
It also calls for a global registry to obtain detailed clinical information on this emerging patient population. UVA Health is partnering with Northwestern University, which is administering the global database.
“The amount of available literature on lung transplantation for CRLD remains sparse,” the authors note.
“Limited experience exists in regard to patients who survive COVID-19 but develop pulmonary fibrosis necessitating consideration for lung transplantation at a later time. Even less is known about patients with preexisting lung disease‚ where COVID-19 exacerbates respiratory failure and leads to potential transplant candidacy.”
Shifting to an Expedited Pretransplant Process
Mannem is proud of UVA Health’s ability to quickly streamline the pretransplant workup from a 3-month to 3-day process when necessary.
This expedited process proved lifesaving in response to otherwise healthy young adults developing acute respiratory failure from severe COVID. It is now being done at UVA Health in approximately 25% of lung transplant candidates, Mannem notes.
PCPs Key as COVID’s Full Impact Yet to Be Felt
While COVID has evolved into what looks more like an upper respiratory virus similar to flu, Mannem predicts it will continue to make an impact for many years to come.
“We are still seeing patients who have true COVID-pneumonia in their lungs upon acute presentation. And when you think about the percentage of patients who had COVID pneumonia early on and progressed to permanent lung damage, so many have yet to have full medical follow up to ensure no lingering pulmonary deficit,” she says.
Primary care providers will likely be the first to uncover these patients.
“It is important for community providers to recognize that patients who have been hospitalized with COVID pneumonia may have some degree of permanent pulmonary impairment. And if that impairment is severe enough to need oxygen to be functional, those patients need to be seen in interstitial lung disease and lung transplant clinics at tertiary care centers,” Mannem says.
Uncovering the Natural History of COVID
At UVA, these patients will receive leading-edge care, and they will already be in a system with transplant expertise if they progress to end-stage lung disease.
They will also have the chance to be part of clinical trials and research registries to better understand this new disease.
UVA Health was among the nation’s first hospitals to create a COVID clinic. Under the leadership of Alex Kadl, MD, MS, a UVA Health critical care pulmonologist, the clinic is studying COVID’s long-term impact.
“We don't yet know the natural history of COVID fibrosis,” Mannem says.
“We see some patients who recover their lung function. But we also see patients, at least based on imaging, progressing to end-stage lung disease. And right now, the only life-saving treatment is transplant.”